DEVELOPMENTS
Health Security is Everyone’s Business: Reflections from the Tackling Deadly Diseases in Africa Programme
Jul 11, 2022
Last month the World Health Organization highlighted the need for “a stronger and more inclusive health emergency preparedness, response, and resilience (HEPR) architecture” in its global architecture concept note. The organization called for better governance, financing, and systems for health security—including taking “a whole-of-society approach for collaborative surveillance, community protection, clinical care, and access to countermeasures.”
The message is loud and clear—health resilience is only possible when everyone is participating in health security.
The Tackling Deadly Diseases in Africa (TDDA) programme—which works across Chad, Cameroon, Côte d’Ivoire, Mali, and Uganda—showed us firsthand why we need a whole-of-society approach to stop future pandemics. Funded by the U.K. Foreign, Commonwealth & Development Office, the project is boosting adherence to the International Health Regulations (IHR), improving community-based disease surveillance, and helping countries to prepare and respond better to health emergencies. TDDA has highlighted that both multisector collaboration and strong civil society engagement are critical to national health security systems.
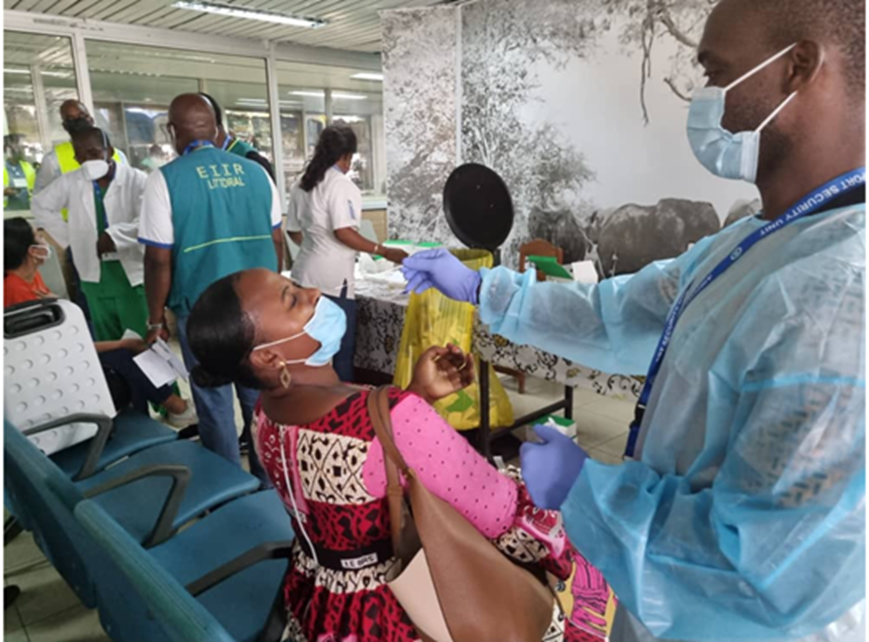
Conducting simulations at the border. Photo: FCDO TDDA.
Why a One Health Approach is Key
Inclusive national health security systems must take a One Health approach. Within TDDA, we are responsible for helping countries strengthen or establish their national One Health platforms, but of course, all countries have different starting points. In Chad, for example, the country started with nothing from a health security perspective. It didn’t have a One Health platform, collaborative One Health activities, or proper coordination between government ministries.
When TDDA began its work in Chad, we started speaking to various ministries (environment, agriculture, health, and others) and brought them all together. We agreed that the government would take the steering wheel in this process, so to speak, while TDDA sat in the passenger seat with a map. We offered technical expertise, but we were there to support—not lead—the way. We asked our government partners what they wanted to achieve, but we didn’t impose our goals upon them. We helped them form a group of One Health champions and write a first One Health governance manual.
Meeting regularly, the champions were soon recognized by the Prime Minister and tasked with helping to coordinate, manage, and support the country’s COVID-19 response. Chad’s One Health champions are now in the final stages of becoming an official, formally recognized, national body. The Prime Minister will personally endorse the One Health platform and a presidential decree is in the pipeline. His support has generated political will for the initiative and helped the entire government understand the importance of the One Health approach in pandemic preparedness and response.
Community awareness campaigns in Chad helped get the word out about COVID-19. Photo: FCDO TDDA.
Why National Health Security Systems Must be Multisectoral
Inclusive national health security systems must also take a multisector approach, incorporating sectors and government departments that traditionally are not included in health security responses. For example, border and immigration forces are essential to health security and a key component of the World Health Organization’s IHR. Through TDDA, we worked with national governments to hold simulation exercises at border crossings in Guinea and Côte d’Ivoire, training border post staff how to manage sick passengers, especially those with highly infectious diseases, such as Ebola. We also developed standard operating procedures on how to carry out cross-border interventions.
In the months following one such simulation, a small Ebola outbreak occurred following cross-border disease transmission from Guinea to Côte d’Ivoire. But the two countries were prepared. They collaborated across sectors, exchanged information, and screened passengers and goods, stopping the Ebola outbreak from getting out of control. In the coming months, TDDA plans to expand simulation exercises and training to border crossings between Chad and Cameroon, in this case focusing on tackling monkeypox.

Civil society groups got involved in Chad. Photo: FCDO TDDA.
Why We Need Civil Society Involvement
In addition to national health security systems, civil society organizations (CSOs) and community-based organizations are critical national health security partners. These organizations can help build trust between communities and governments—bridging gaps between remote communities and state institutions, and supporting essential services in hard-to-reach areas. CSOs also foster social accountability by encouraging governments to respect commitments, share information, and include the more neglected parts of populations. CSOs tend to be accountable to their own constituencies and the communities they serve, creating greater trust and collaboration between communities and governments.
Within TDDA, civil society groups have emerged as dedicated partners in responding to COVID-19, for example. The project initially urged CSOs into a “policing” role to demand government accountability and transparency regarding health security and IHR commitments. In many countries, this brought civil society in conflict with the government and exacerbated sometimes tense relationships. However, as the pandemic developed, TDDA changed tactics. Governments were severely stretched; they had emergency response coordination needs to meet, and enormous misinformation and vaccine hesitancy issues to combat. It quickly became apparent that civil society and community groups would be more effective as active partners, rather than as policemen. Groups began working with the governments to combat COVID-19 misinformation, run vaccination campaigns, and identify communities that could be particularly susceptible to COVID-19 outbreaks or false information.
Across Côte d’Ivoire and Uganda alone some 12,000 people were sensitized to COVID-19 risks and equipped with accurate, timely information on the pandemic and emergency health services, and thousands more have been vaccinated against COVID-19. Supporting groups with financing and institutional capacity development, while encouraging them to act as government partners, can build stronger democracies and improve health security systems in the long term.
Government ministries, development agencies, local authorities, and civil society each play a unique role in tackling health security challenges. Keeping our societies safe from health emergencies requires everyone’s participation and collaboration. Health security is everyone’s business.
Omer Njajou is the Technical Lead for International Health Regulations for TDDA and Claude Cafardy is the Technical Lead for Governance and Accountability for TDDA.