DEVELOPMENTS
How to Design Nutrition Programs to Increase Health Equity
Jan 12, 2022
Good nutrition is important for everyone—but for the most vulnerable people, healthy diets can mean the difference between life or death. To design effective nutrition programs, international development practitioners need to understand what defines people as vulnerable, what causes that vulnerability, and what to do about it. Recent guidance on Improving How FCDO Reaches Those Most-at-risk of Malnutrition, drafted by DAI for the U.K. Foreign, Commonwealth & Development Office (FCDO), sheds light on these issues.
Malnutrition occurs when people have deficiencies, excesses, or imbalances in the food they eat that results in poor growth, limited development, or impairment. According to the World Health Organization, there are four periods in life when people are most nutritionally vulnerable: the first 1,000 days (pregnancy to age 2), which is the most critical; early childhood (ages 2 to 5), when health and dietary behaviors begin to form; middle childhood (5 to 9), when those behaviors become habits; and adolescence (10 to 19), the second-fastest stage of growth and development in the life cycle, when habits solidify.
Nutritional vulnerability increases when people cannot access nutritious diets, health services, nurturing care, or adequate water and sanitation. Vulnerability also increases when people are marginalized through factors such as poverty, gender inequity, violence, environmental toxins, climate change, or poor mental health.
Understanding who is most at risk, nutritionally, starts by understanding who is most physiologically vulnerable and then looking at the social, economic, and cultural factors they are facing. “Physiologically, a person’s first 1,000 days, from the time of conception to two years of age, are the most critical for growth and development,” says Abigail Ramage, Senior Practice Specialist for Global Health at DAI. “Factors like poverty, disability, and social exclusion, of mothers in particular, are social determinants of health that drive nutritional vulnerability,” she says, citing the FCDO guidance document.
The guidance highlights the multidimensional nature of nutrition, explaining that multiple intersecting factors increase vulnerability. She says: “The tricky thing is that there are so many underlying determinants to good nutrition—education levels, access to a range of foods, cultural norms. It is very difficult to isolate a cause. We must look at the whole context including how the social impacts the physical.”
Geographic and environmental factors can exacerbate vulnerability, adds Stephen Rahaim, Senior Global Practice Leader for Market Solutions in DAI’s Global Health team. “In Bangladesh, for example, living in flood-prone regions of the country significantly affects people’s ability to farm and grow food, affecting supply chains, livelihoods, and market access to food, making them more vulnerable. Additionally, internal and cross-border instability and displacement, like that currently affecting the Rohingya population, can increase food insecurity and decrease food production.”

Bangladeshis live in flood-prone regions. Photo: USAID Bangladesh.
Tackling the Multiple Dimensions of Malnutrition
Because nutrition is multidimensional, solutions must be too. Strong health programming, nutrition-focused or otherwise, starts by authentically engaging communities in identifying their problems and needs, working within existing systems, empowering both women and men, and improving transparency in resource allocation and decision making. Reaching the most vulnerable means working with health and community systems in partnership.
1. Talk to People
“The first step of any intervention is to understand, talk to people, and bring them into the program design from the start,” says Paula Quigley, Technical Lead for Reproductive, Maternal, Newborn, Child and Adolescent Health, Evidence and Learning at DAI. “People from particularly marginalized groups tend to have multiple problems or vulnerabilities; they may be exceptionally poor, socially excluded, or have a disability. Understanding the community’s particular vulnerabilities is key.”
Quigley tells a story from her community health work in Zambia, on the Moblising Access to Maternal Health Services (MAMaZ), where she and her colleagues found an entire community blacklisted and shunned by the surrounding groups for various reasons. They were cut off from services, highly vulnerable, and in the absence of a comprehensive community engagement process would have missed out completely on the MAMaZ program’s offerings.

Interventions in Zambia focused on increasing access to health services. Photo: Medicines for Malaria Venture MAMaZ.
Social norms, cultural beliefs, and practices are intrinsically tied to knowledge, attitudes, and behaviors that can perpetuate nutritional inequities. A thoughtful understanding of how behavioral norms affect daily life for people can ensure interventions are appropriately nuanced and based on evidence.
For example, in Bangladesh, the Policy LINK project is working with highly vulnerable communities to revitalize sustainable agriculture to improve their food security and nutritional status. The project is underpinned by a rigorous co-creation process that engages stakeholders at regional, community, and national levels to understand local motivations, attitudes, and behaviors. Co-creation and participatory stakeholder engagement are critical to designing interventions that stick.
2. Work with What’s There
“If something exists, even only on paper, we will always aim to strengthen that and build on it rather than develop something new.” That’s the principal Quigley and DAI work from—to work within systems wherever possible, rather than creating new ones. Many countries have national community health programs, with community health workers or volunteers and health facilities. Supporting government systems, no matter how nascent they are, helps ensure interventions are sustainable.
In the MAMaZ program, the team worked within the national health system to provide safety nets for pregnant women and new mothers. Local volunteers led safe motherhood groups and were visited regularly by community health workers and community facilitators. Health workers were supported by local health facilities and facilities were supported by district health authorities, ensuring the program was strengthened by government public health structures.
3. Improve Gender Equality
In communities with more traditional or patriarchal structures, ensuring women and men are incorporated in decision making and program development is vital. Pregnant and nursing women are some of the most physiologically vulnerable people, and often the most socially vulnerable because of behavioral norms. Improving gender equality can improve the health and wellbeing of the entire community.
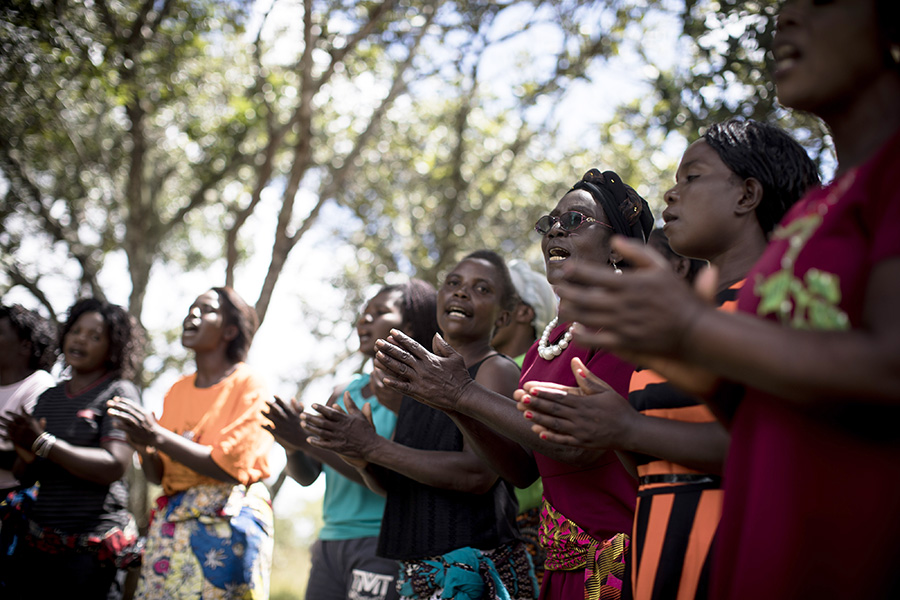
Interventions in Zambia also focused on increasing the number of women involved. Photo: MAMaZ.
“Improving gender equality starts with creating more awareness of inequality,” says Quigley. Within the MAMaZ project, Quigley and her team educated both men and women about maternal and newborn health, the impact of gender-based violence, and the importance of safe pregnancy and motherhood. Men in the community were asked to volunteer time for emergency transport schemes—ferrying women to medical services by boat, bicycle, or taxi, for example—thereby giving them responsibility and co-ownership in the maternal health initiative.
As men came to better understand how their actions affected women around them, they began to change, and health improved. Through its empowerment approach, the project reported an 88 percent decrease in gender-based violence and a 27 percent increase in the number of babies delivered by a skilled birth attendant.
4. Track the Money
Improving how funding is tracked, as it moves from national health systems to the community level, helps ensure the most vulnerable people can access healthcare. Better financial transparency and accountability through internal controls, auditing, and budgeting procedures means money is more likely to reach the people at the “last mile” of a health system. For example, in Malawi, under the Accelerating Support to Advanced Local Partners project, health authorities have been able to hire hundreds more health workers in the community because of better financial and human resource systems.
Rahaim says “improving the targeting of social benefits” can also improve the equity of access to services. For example, in Bangladesh, politically appointed local leaders are responsible for identifying who is most vulnerable in order for them to qualify for social benefits. The selection of community members, therefore, is often politically motivated, rather than being criteria- and needs-based. Objective vulnerability frameworks allow those most in need to receive social benefits that can improve their ability to access nutritious foods and appropriate healthcare services, making social benefits more impactful.
Reaching those most in need requires programs built on genuine engagement, determined support to existing systems, a deep understanding of cultural barriers and behavioral triggers, and financial transparency. Whether it is improving agricultural practices in Bangladesh, upgrading maternal health in Malawi, or developing guidance on reaching the underserved, understanding people, working collaboratively, and taking the time to seek out and support the most vulnerable means our programs can make the world a more equitable place.
Megan Howe is a Senior Communications and Knowledge Management Advisor for DAI’s Global Health practice. Email Megan with questions or comments.